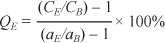Radiologia Brasileira - Publicação Científica Oficial do Colégio Brasileiro de Radiologia
AMB - Associação Médica Brasileira CNA - Comissão Nacional de Acreditação
 Vol. 42 nº 2 - Mar. / Apr. of 2009
Vol. 42 nº 2 - Mar. / Apr. of 2009
|
ORIGINAL ARTICLE
|
|
Comparative study on imaging quality in PET acquisition modes: validation of a protocol for reducing the radiation dose |
|
|
Autho(rs): Solange Amorim Nogueira, Henrique Manoel Lederman, Jairo Wagner, Lilian Yuri Yamaga, Marcelo Livorsi da Cunha, Marcelo Buarque de Gusmão Funari |
|
|
Keywords: PET/CT, Imaging quality, 2D mode, 3D mode, 18F-FDG, Dose reduction |
|
|
Abstract:
IMaster, Biomedical Coordinator, Unit of Nuclear Medicine at Hospital Albert Einstein, São Paulo, SP, Brazil
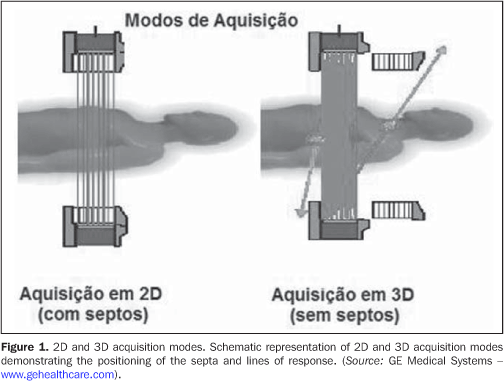
INTRODUCTION Positron emission tomography/computed tomography (PET/CT) was introduced in 1998 and has had a remarkable impact on the diagnostic medicine, particularly in the field of oncology. The major advantage of this imaging method is the property of producing both morphological and functional images of pathological processes. The glucose analog F-18-fluorodeoxy-glucose (FDG-18F) is a marker of cell metabolism that can be non-invasively detected by PET(1). The combination of this technique with radiographic tomography allows the fusion of metabolic and anatomical images resulting in a precise localization of pathological processes, allowing the staging, monitoring and management of the disease, providing higher specificity, sensitivity and accuracy to the patient assistance strategy(2). However, both procedures involve patients exposure to radiation, a critical issue for pediatric patients, so there is interest in developing a protocol capable of minimizing radiation exposure without impairing the diagnosis(3,4). The effective dose in patients submitted to PET/CT scans who have received activities between 300 MBq and 370 MBq is approximately 25 mSv, 10 mSv of which result from the administration of FDG-18F or 0.027 mSv/MBq. So, any reduction in the activity administered in PET implies a proportional reduction of the effective dose delivered to the patient(5,6). The research of techniques which allow the reduction of radiation doses has a great relevance in studies developed in the area of oncology where the patient is followed-up with a series of radiological studies. Positron emission tomography can be performed through two acquisition modes: 2D and 3D as shown on Figure 1.
The 2D acquisition mode utilizes tungsten septa placed under the detectors. These septa act as antidiffusion grids utilized in radiology. They cause a reduction in the photons incidence angle, resulting in a decrease of up to 15% in the rate of false events produced by scattering photons. As a result, the images contrast resolution is improved although the equipment count rate performance decreases so the administration of a higher radioactivity is required for images acquisition(7,8). In the 3D acquisition mode, the septa are retracted and an electronic collimation of the detected coincidences is utilized, resulting in up to six-fold higher count rates. As a result, there is an increase in the equipment sensitivity, allowing a reduction both in the radioactivity administered to the patient and in the acquisition time. On the other hand, as a disadvantage, the increase in the count rate receives the contribution of false coincidences (random and scattering events), which cause a reduction in the images contrast resolution(7,8). Centers where PET/CT scans are performed with the 2D acquisition mode replace this protocol by the 3D mode as a strategy to reduce radiation doses for allowing the administration of lower radiopharmaceutical activity. In this context, studies aimed at demonstrating the appropriateness of 3D acquisition mode to preserve the image quality with the administration of lower radiotracer activity are important for the clinical routine. The present study is aimed at evaluating whether images obtained with the 3D acquisition mode with two minutes (3D-2-min) and four minutes (3D-4-min) and lower FDG-18F activity, present the same image quality provided by the 2D acquisition mode (2D-4-min), which is usually utilized as a standard in the department, and, based on this evaluation, validating a new protocol of 3D acquisition mode to replace the 2D mode, reducing the activity and, consequently, the radiation dose delivered to the patients, without a loss in the image quality.
MATERIALS AND METHODS The present study was developed with a Discovery ST PET/CT equipment (General Electric Medical System; Milwaukee, USA) utilizing crystalline bismuth germanate (BGO)(9,10). The experimental method employed image quality tests according to the 2001 version of the protocol of the National Electrical Manufacturers Association Standards (NEMA) (NU 2-2001). A phantom (NEMA/IEC 2000; Biodex) was utilized to simulate a human thorax both in shape and size. This phantom includes six spheres with different diameters (1 cm, 1.3 cm, 1.7 cm, 2.2 cm, 2.8 cm, 3.7 cm) transversely positioned on a circumference (23 cm in diameter), and a cylinder (5 cm in diameter) positioned on the center(10). In compliance with the protocol for testing image quality, the phantom and the four smaller spheres were filled with radioactive material at different concentrations, and the cylinder, with cotton to simulate the pulmonary parenchyma. With this arrangement, the authors could identify "hot" (four spheres) and "cold" (two spheres and the cylinder) images in relation to the background (bg) radiation. The activities utilized in the phantom components were in compliance with the NEMA manual(10). A NEMA phantom for scatter test is utilized to include information from scatter photons of other regions. This phantom is comprised of a cylinder with 70 cm in length and 20 cm in diameter, and a central canal through which passes a plastic tube filled with radioactive material. A whole-body study can be simulated with this arrangement(10). The 3D acquisitions were performed two hours after the 2D acquisitions to take advantage from the 18F radioactive decay resulting in a reduction to about one-half of the initial activity. The images acquired were reconstructed on a Xeleris workstation (GEMS), by means of interactive ordered subset expectation maximization (OSEM), with 21 subsets and two iterations for the 2D mode, and Fourier rebinning-OSEM (FORE-OSEM) with 24 subsets and three iterations for the 3D mode. Twenty-seven simulations were performed over a one-year period. In this period, the equipment was evaluated by means of daily, weekly and quarterly quality control tests, according to the NEMA recommendations. The results of these tests are in compliance with the manufacturer standards. The set of images resulting from each simulation were qualitatively analyzed on the workstation by three experienced radiologists who did not know the acquisition modes utilized. Each observer attributed a score 1 when at least one of the spheres was not identified or in cases where the image was dubious, or 2 for clearly visible spheres. The contrast value for the smallest sphere of each simulation was found through the image quality test of the NEMA protocol. It is defined as the relation between the activity calculated by the count of the designed region of interest (ROI) and the real activity. The contrast value in the "hot" spheres is calculated according to the following formula(11):
where: CE = counts in the area corresponding to the smallest sphere; CB = count in the area corresponding to the bg; aE = activity concentration in the "hot" sphere; aB = activity concentration in the bg. In the present study, only the contrast values for the smallest (1 cm) "hot" spheres were utilized. Initially, all the data collected were descriptively analyzed. Subsequently, some summary measures, such as mean, standard deviation, among others, were calculated, and boxplots were constructed for quantitative variables(12). The qualitative variables (observers' scores) were analyzed through the calculation of absolute and relative frequencies(12). The inferential analyses performed to confirm or contradict the evidences found by the descriptive analysis were: block variances analysis, besides Bonferroni comparison, as necessary(13); and estimation of generalized kappa coefficient of agreement(14). A level of significance á corresponding to 5% was utilized to draw conclusions through the inferential analyses. The data were appropriately stored in an Excel 2000 worksheet for Windows, and the software Statistical Package for Social Sciences (SPSS) version 11.0 for Windows was utilized for statistical analysis.
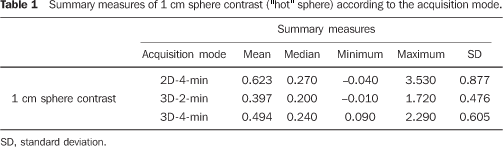
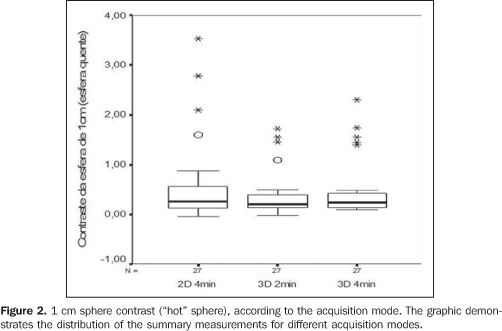
RESULTS Data regarding contrast observed in the 1 cm sphere through the three acquisition modes are shown on Table 1 and Figure 2.
The inferential results demonstrated that the mean 1 cm sphere contrast ("hot" sphere) is higher in the 2D acquisition mode (p = 0.014). Table 2 shows the comparison of mean values of the different acquisition modes for the 1 cm sphere contrast.
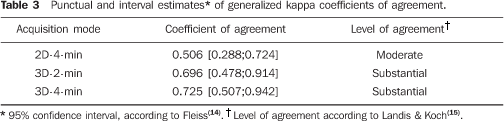
The evaluation of the interobserver agreement as regards the spheres visualization was also included in the present study. The rates of interobserver agreement in relation to the 2D-4-min, 3D-2-min and 3D-4-min acquisition modes were, respectively, 63.0%, 77.8% and 88.9%. Generalized kappa coefficient was estimated for quantifying the level of interobserver agreement. Table 3 with these estimates demonstrates a good interobserver agreement.
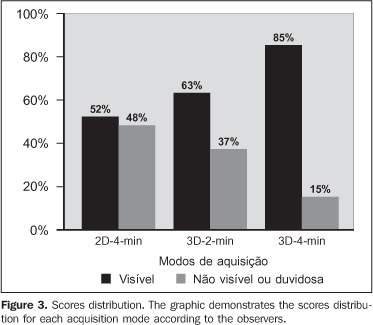
The images obtained were individually classified by each of the observers into visible (score 2) or non-visible (score 1). This qualitative evaluation was performed for the different acquisition modes. The scores distribution among the acquisition modes is shown on Figure 3, where one can observe that the percentage of times where all the spheres were identified was highest with the 3D-4-min acquisition mode. Additionally, the number of times where there was difficulty in visualizing the spheres with the 3D-4-min mode was three-fold lower than with the 2D-4-min mode and two-fold lower than with the 3D-2-min mode.
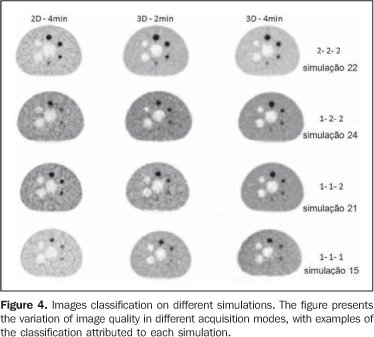
Correlation between image quality and acquisition modes considering the category variables (visible or non-visible spheres) was determined by consensus among the observers based on a single score for the three acquisition modes on each simulation. The results of this distribution are shown on Table 4 and the image classification as well as their respective scores are shown on Figure 4.
These data were evaluated through the generalized kappa test whose results demonstrate a moderate correlation among the three acquisition protocols: 0.444 [0.227; 0.662].
DISCUSSION Nuclear medicine services with BGO-based PET-CT scanners preferentially utilize the 2D acquisition mode which provides better image quality. However, a higher FDG-18F activity is required in this acquisition mode and, consequently, the patient receives a higher radiation dose. Studies comparing 2D and 3D acquisition modes have been developed aiming at finding a balance in the utilization of these technological resources with dose optimization. The 2001 version of the NEMA protocol for testing image quality was designed to simulate whole-body studies with both acquisition modes, and for this reason this protocol was utilized in the present study so that the patients were not unnecessarily irradiated. The analysis of the tests results demonstrated that the 2D acquisition mode provides a better contrast resolution for "hot" spheres". A similar result has been observed by Bettinardi et al.(16) and Mawlawi et al.(9), according to studies published in 2004, where these authors evaluated the performance of the same PET/CT system utilized in the present study, considering this equipment as efficient with both acquisition modes. A relevant issue to be considered is that the patient bodily mass can influence the image quality. A study developed by El Fakhri et al.(17) has concluded that BGO-based PET/CT scans produce similar results in the detection of lesions with different sizes with both 2D and 3D acquisition modes, but the 3D mode presents a better performance in the detection of lesions in patients with body mass index < 33; on the other hand, the 2D mode is better for patients with body mass index > 34. A study published by Visvikis et al.(18) in 2005 also demonstrated that in studies performed with BGO-based equipment the images quality is similar with both the 2D and 3D acquisition modes. In this study, the author has observed a correlation among image quality, patient's body weight and acquisition time, and has demonstrated that the increase in the patient weight leads to a progressive loss of image quality in both acquisition modes, but particularly with the 3D mode in patients weighting more than 70 kg. Lodge et al. have compared 2D and 3D acquisition modes in a PET scanner with lutetium oxyorthosilicate crystal (LSO) and have observed that the 3D acquisition mode presented a better performance because of the crystal characteristics, allowing a reduction of dose and acquisition time(19). Although LSO-based equipment is more appropriate for 3D-acquisition, increased patient weight leads to a loss in the image quality, so an extended acquisition time is required to compensate this problem(20). Bettinardi et al. have evaluated the Discovery STE with a new configuration of BGO crystals, and have concluded that the greatest advantage of the 3D acquisition mode is the increase in the system's sensitivity and the utilization of new reconstruction algorithms allowing an improvement in the images quality, in the capability to detect lesions and in the accuracy of the method as compared with the 2D acquisition(21). The results of the present study demonstrated a moderate correlation among the 2D-4-min, 3D-2-min and 3D-4-min acquisition modes as regards the visualization of "hot" spheres, generalized kappa coefficient = 0.444 [0.227;0.662], highlighting the 3D-4-min acquisition mode, where all the spheres were visible for the highest number of times (85%). The rate of interobserver agreement was higher with the 3D-4-min than with the other acquisition modes (88.9%), with a generalized kappa coefficient = 0.725 [0.507;0.942]. These results are significant because they indicate that the 3D acquisition mode can be utilized with BGO-based PET/CT scanners for patients whose thorax dimensions are similar to the phantom's. Based on the results of the present study, the authors could establish protocols with lower FDG-18F activity, which will be very useful in the case of pediatric patients.
CONCLUSION The experimental study has demonstrated that there is no loss in imaging quality with the utilization of the 3D acquisition mode with half the administered activity The 3D-4-min acquisition mode has allowed the spheres visualization in the majority of tests, so this technique can be utilized as a strategy to reduce the FDG-18F activity delivered to patients with a biotype similar to the phantom. The results of the present study suggest that the proposed 3D-4-min acquisition mode with BGO-based PET/CT scanners will allow a reduction in the radiation activity and, consequently, lower irradiation doses to the patient, affecting especially the application of PET in pediatrics.
REFERENCES 1. Lomeña F, Soler M. Clinical application of PET. Braz Arch Biol Technol. 2005;48(no. spe 2):179-83. [ ] 2. Townsend DW, Beyer T, Blodgett TM. PET/CT scanners: a hardware approach to image fusion. Semin Nucl Med. 2003;33:193-204. [ ] 3. Hahn K, Pfluger T. Is PET/CT necessary in paediatric oncology? Against. Eur J Nucl Med Mol Imaging. 2006;33:966-8. [ ] 4. Stauss J, Franzius C, Pfluger T, et al. Guidelines for 18F-FDG PET and PET-CT imaging in paediatric oncology. Eur J Nucl Med Mol Imaging. 2008;35:1581-8. [ ] 5. Brix G, Lechel U, Glatting G, et al. Radiation exposure of patients undergoing whole-body dual-modality 18F-FDG PET/CT examinations. J Nucl Med. 2005;46:608-13. [ ] 6. Cálculo da dose efetiva. [acessado em 30 de julho de 2008]. Disponível em: http://www.doseinforadar.com/RADARDoseRiskCalc.html [ ] 7. Townsend DW. Physical principles and technology of clinical PET imaging. Ann Acad Med Singapore. 2004;33:133-45. [ ] 8. Schöder H, Erdi YE, Larson SM, et al. PET/CT: a new imaging technology in nuclear medicine. Eur J Nucl Med Mol Imaging. 2003;30:1419-37. [ ] 9. Mawlawi O, Podoloff DA, Kohlmyer S, et al. Performance characteristics of a newly developed PET/CT scanner using NEMA standards in 2D and 3D modes. J Nucl Med. 2004;45:1734-42. [ ] 10. GE Healthcare. DST PET-CT NEMA test procedures, applicable to Discovery ST. Direction 5159176-100, Revision 2. Walkesha: General Electric Company; 2006. [ ] 11. National Electrical Manufacturers Association. Standards Publication NU-2-2001: performance measurements of positron emission tomography. Rosslyn: National Electrical Manufacturers Association; 2001. [ ] 12. Bussab WO, Morettin PA. Estatística básica. 5ª ed. São Paulo: Saraiva; 2006. [ ] 13. Neter J, Kutner MH, Nachtsheim CJ, et al. Applied linear statistical models. 4th ed. Boston: Irwin; 1996. [ ] 14. Fleiss JL. Statistical methods for rates and proportions. 2nd ed. New York: John Wiley; 1981. [ ] 15. Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33:159-74. [ ] 16. Bettinardi V, Danna M, Savi A, et al. Performance evaluation of the new whole-body PET/CT scanner: Discovery ST. Eur J Nucl Med Mol Imaging. 2004;31:867-81. [ ] 17. El Fakhri G, Holdsworth C, Badawi RD, et al. Impact of acquisition geometry and patient habitus on lesion detectability in whole body FDG-PET: a channelized hotelling observer study [abstract]. Nuclear Science Symposium Conference Record, 2002 IEEE. 2002;3:1402. [ ] 18. Visvikis D, Griffiths D, Costa DC, et al. Clinical evaluation of 2D versus 3D whole-body PET image quality using a dedicated BGO PET scanner. Eur J Nucl Med Mol Imaging. 2005;32: 1050-6. [ ] 19. Lodge MA, Badawi RD, Gilbert R, et al. Comparison of 2-dimensional and 3-dimensional acquisition for 18F-FDG PET oncology studies performed on an LSO-based scanner. J Nucl Med. 2006;47:23-31. [ ] 20. Halpern BS, Dahlbom M, Quon A, et al. Impact of patient weight and emission scan duration on PET/CT image quality and lesion detectability. J Nucl Med. 2004;45:797-801. [ ] 21. Bettinardi V, Mancosu P, Danna M, et al. Two-dimensional vs three-dimensional imaging in whole body oncologic PET/CT: a Discovery-STE phantom and patient study. Q J Nucl Med Mol Imaging. 2007;51:214-23. [ ] Received August 10, 2008. * Study developed at Hospital Israelita Albert Einstein, in a partnership with Universidade Federal de São Paulo/Escola Paulista de Medicina (Unifesp/EPM), São Paulo, SP, Brazil. |
|
Av. Paulista, 37 - 7° andar - Conj. 71 - CEP 01311-902 - São Paulo - SP - Brazil - Phone: (11) 3372-4544 - Fax: (11) 3372-4554