Radiologia Brasileira - Publicação Científica Oficial do Colégio Brasileiro de Radiologia
AMB - Associação Médica Brasileira CNA - Comissão Nacional de Acreditação
 Vol. 40 nº 2 - Mar. / Apr. of 2007
Vol. 40 nº 2 - Mar. / Apr. of 2007
|
ORIGINAL ARTICLE
|
|
Predictive values of bi-rads categories 3, 4 and 5 in non-palpable breast masses evaluated by mammography, ultrasound and magnetic resonance imaging |
|
|
Autho(rs): Decio Roveda Junior, Sebastião Piato, Vilmar Marques de Oliveira, José Francisco Rinaldi, Carlos Alberto Pecci Ferreira, Eduardo de Castro Faria Fleury |
|
|
Keywords: BI-RADS, Breast cancer, Mammography, Predictive value |
|
|
Abstract:
IProfessor Instructor, Director for the Service of Diagnostic Imaging of the Department of Clinical Medicine of Faculdade de Ciências Médicas da Santa Casa de São Paulo, São Paulo, SP, Brazil
INTRODUCTION It is unquestionable that the programs of mammographic breastcancer screening have caused a significant decrease in themortality by this disease thanks to the early diagnosis in aconsiderable number of cases, as evidenced by several clinicalinvestigations(1–6). However, the mammographic screening started being complementedby a great number of unnecessary biopsies, since a considerablepart of lesions considered as suspect of malignancy have beenfound to be benign. Of 1,000,000 women submitted to breast biopsyin the USA as a result of abnormal mammographic findings inbreast cancer screening programs, 700,000 to 850,000 presentednegative results(7). Aiming at improving the effectiveness of breast cancerscreening programs, with an increase in quality of reports issuedby radiologists; and recognizing the necessity of providingmeaningful and unambiguous reports to allow a reliable dataacquisition, the American College of Radiology, in acollaborative effort with the American Cancer Institute andAmerican College of Surgeons, in 1992 developed a system for notonly classifying mammographic images, but also for structuringreports by means of lesions description and standardization ofconclusions, and suggesting a course of action to be adopteddepending on the final findings classification. The result of such collaborative effort is the Breast ImagingReporting and Data System (BI-RADS™), contemplating not onlya classification of outcomes, but also the recommendation of aspecific course of actions which, if adopted, will allow a higherefficacy of programs for early breast cancer detection. Thesystem includes an introduction, a breast imaging lexicon and areporting standardization and diseases coding system, besides areliable methodology for outcomes monitoring andfollow-up(8). Based on a descriptive lexicon of radiological lesions, thesystem classifies the findings into seven categories, aiming atfacilitating the decision making on a specific course of actionby physicians in face of abnormal image findings. On its fourthand latest issue released in December 2003, the BI-RADS Atlas,formerly restricted to the area of mammography, extends thestandardization to the areas of ultrasonography and magneticresonance imaging(8). The BI-RADS introduction raised the radiologists and breastspecialists concern about the predictive values of categories 3,4 and 5, aiming at improving the management of abnormal,non-palpable findings. BI-RADS classification Category 3 – A finding in this category presents a high probability of benignity. However, considering a very low possibility of malignancy, a short interval follow-up is recommended for evaluation of the lesion stability (Figure 1). Category 4 – The lesions do not present any morphological characteristics typical of cancer, although with high probability of malignancy. The images raise sufficient concern to suggest a biopsy (Figure 2). Category 5 – Lesions with morphological characteristics highly suggestive of malignancy (Figure 3). A review of the literature regarding the predictive values ofBI-RADS categories 3, 4 and 5 has demonstrated the inexistence ofstudies on mammography exclusively related to non-palpable breastmasses. As regards breast ultrasound, Hong et al.(9)have studied 403 solid breast lesions, aiming at determining thepositive predictive value (PPV) and negative predictive value(NPV) of these findings, according to echographic characteristicsand respective histological diagnoses described in the newBI-RADS lexicon. They have found 141 (35%) positive cases withcharacteristics described by BI-RADS as malignant demonstratinghigh PPV. Solid lesions with spiculated margins presented 86% PPV(19 of 22); irregular lesions, 62% PPV (102 of 164); lesions witha non-parallel orientation in relation to the costal grid, 69%PPV (75 of 109). As regards NPV, high values also have beenobserved for findings described by BI-RADS, such as circumscribedmargins in 90% (160 of 178), parallel orientation in relation tothe costal grid in 78% (228 of 294), and oval shape in 84% (200of 237). These results show that the characteristics described inthe new BI-RADS sonographic lexicon may be useful fordifferentiating between malignant and benign solid lesions. Gokalp and Topal(10) have developed a studyaiming at analyzing magnetic resonance imaging as method forevaluating supposedly benign lesions classified as BI-RADScategory 3. They have studied 56 lesions present in 43 femalepatients, comparing the studies with the respective histologicalresults, and calculating sensitivity, specificity and predictivevalues. The values found for lesions classified as probablybenign were: 100% for sensitivity, 94.6% for specificity, 33.3%for PPV, and 100% for NPV, allowing us to conclude that thesystem may be useful in a conservative management of alterationsclassified as BI-RADS category 3. A similar study developed by Sadowski andKelcz(11) aimed at determining the chance ofmalignancy for breast lesions classified as probably benign, hasretrospectively evaluated 473 patients submitted to magneticresonance imaging in the period between March 1994 and March2002, and observed that 17% (79 of 473) were classified asprobably benign. Of this group, 68 patients were followed-upduring a minimum two-year period, and 6% (4 of 68) presentedbreast cancer in 14 to 18 months subsequent to the initialassessment. This study has led us to the conclusion that patientsevaluated by means of magnetic resonance imaging and classifiedas BI-RADS category 3 are at higher risk for breast cancer thanthose evaluated by mammography in the same category. The present study was aimed at evaluating the PPV and NPV ofBI-RADS categories 3, 4 and 5 in non-palpable breast massesevaluated by mammography, ultrasound and magnetic resonanceimaging.
MATERIALS AND METHODS Twenty-nine dossiers of patients with mammographic findings ofnodular lesions in BI-RADS categories 3, 4 and 5 were evaluated.One of the patients presented with findings in both breasts, sothe number of lesions increased to 30. The patients also hadtheir lesions evaluated by ultrasound and magnetic resonanceimaging. The following exclusion criteria were taken into considerationfor the casuistic selection: 1) abnormal mammographic findingsvisualized on a single view; 2) abnormal findings withsuperficial or retroareolar localization; 3) patients withfindings classified as BI-RADS categories 0, 1, 2 and 6 oncomplementary ultrasound and magnetic resonance imaging; 4)patients previously submitted to radiotherapy, chemotherapy orhormone therapy. The mammographic examinations were performed in a Philips M3000 model equipment, with 0.1 and 0.3 mm microfocus, molybdenumanode, rhodium filter and automatic exposure meter. All the patients were submitted to bilateral examination oncraniocaudal and mediolateral oblique, 25° angle views;additional views with spot-compression and image magnificationwere made as necessary. The images were analyzed in a dark room by means of a4-compartment negatoscope with the aid of a magnifying glass, andreports were elaborated by one of the authors of the presentstudy, who is radiologist and specialist in breast imaging, andby another radiologist also experienced in breast imaging. All the images were rated according to characteristics of thefindings of non-palpable masses, based on the definitions ofBI-RADS categories 3, 4 and 5. Ultrasound studies were performed in a digital model 1500 HDIequipment, with a 7.5–10.0 MHz linear transducer. All the patients underwent bilateral examination, with radial,anti-radial and transverse scanning technique, and thedocumentation was elaborated in digital file. The sameradiologists responsible for the mammographic reports elaborationperformed the examinations. All the sonographic images were classified according tocharacteristics of the findings of non-palpable masses, based onthe definitions of BI-RADS categories 3, 4 and 5. The magnetic resonance imaging studies were performed in a 1.0tesla Philips, T10 NT model equipment, with a breast coil. Thesame radiologists responsible for the mammographic reportselaboration performed the examinations. Initially, sagittal, T2-weighted sequences were performed; andafter, axial and sagittal, T1-wieghted sequences at a 5 mminterval, before and after intravenous paramagnetic contrastinjection. The contrast agent utilized was gadolinium-diethylenetriaminepentaacetic acid (Gd-DTPA), administered in 10 ml bolus. The images were analyzed by the same radiologists andclassified according to characteristics of the findings ofnon-palpable masses, based on the definitions of BI-RADScategories 3, 4 and 5. All of the non-palpable lesions were submitted to wire-guidedsurgical biopsy(12). After the radiologicalcontrol, the specimens were sent for histopathological study, inplastic recipients containing formol at 10%, positioning theguide wire the nearest possible of the lesion for an easieridentification. The biopsy slides reading was performed in an ordinary opticalmicroscope. The reports with results were issued in compliancewith the World Health Organization standards. PPV and NPV were calculated according to the methodology included in the BI-RADS chapter 5 – "Results Monitoring". In this methodology, the classification of images and respective anatomopathological results are taken into consideration (Table 1).
PPV calculation – PPV is defined as the percentage ofall the biopsies performed because of abnormal mammographicfindings which have resulted in a diagnosis of cancer. The PPVcalculation in the different BI-RADS categories was made by meansof the following equation: True-positive (TP) / true-positive (TP) + + false-positive (FP) NPV calculation – The NPV is defined as the percentageof all the biopsies performed because of abnormal mammographicfindings which have not resulted in a diagnosis of cancer. TheNPV calculation in the three BI-RADS categories was made by meansof the following equation: True-negative (TN) / true-negative (TN) + + false-negative (FN) Statistical analysis – The statistical analysis wasperformed after the descriptive analysis tabulation of dataincluded in explanatory tables and graphs. For testing thegroups' homogeneity as regards (positive and negative) predictivevalues, the Fisher's exact test was employed for expectedfrequencies of < 5. The null hypothesis rejection level wasset at 5% (p < 0.05). The kappa concordance index wasutilized for evaluating the concordance of the classification ofmammographic, sonographic and magnetic resonance imaging findingswith the histopathological results(13).
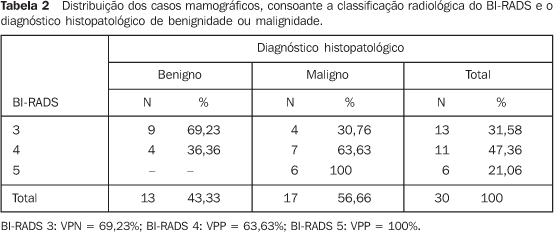
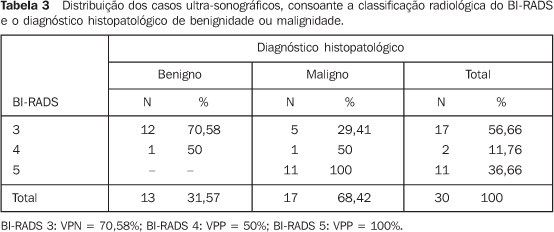
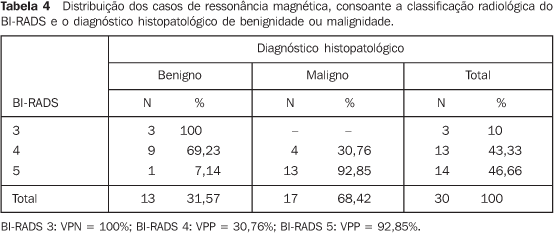
RESULTS The data indicate a predominance of benign results in patientswith BI-RADS category 3 findings in mammographic (69.23%),sonographic (70.58%) and magnetic resonance imaging (100%)evaluations. Among patients with BI-RADS category 4 findings, the cases ofhistopathological malignancy increased progressively onmammographic, sonographic and magnetic resonance imagingevaluations, representing respectively 63.63%, 50% and 30.76%. Onthe other hand, cases of histopathological benignity in BI-RADScategory 4, constituted respectively 30.76%, 50% and 69.23%. A similar phenomenon was observed in the evaluation ofpatients with results in the BI-RADS category 5. A progressiveincrease is observed on mammographic, sonographic and magneticresonance imaging evaluations, representing 100% in the first twomodalities, and 92.85% in the latest. On the other hand, thecases of histopathological benignity decreased to 0% in category5 for mammographic and sonographic evaluations, and 7.15% formagnetic resonance imaging. For the mammographic analysis of 13 cases of supposedly benignfindings included in category 3, 10 cases presentedhistopathological negative results for malignancy, showing 69.23%NPV. For the sonographic analysis of 17 cases of supposedlybenign findings included in category 3, 12 presentedhistopathological negative results for malignancy, showing 70.58%NPV. For the analysis by magnetic resonance imaging of threecases of supposedly benign findings included in category 3, allthe cases presented histopathological negative results formalignancy, showing 100% NPV. For the mammographic analysis of 11 cases of supposedlymalignant findings included in category 4, seven cases presentedhistopathological positive results for malignancy, showing 63.63%PPV. For the sonographic analysis of two cases of supposedlymalignant findings included in category 4, one case presentedhistopathological positive results for malignancy, showing 50%PPV. For the analysis by magnetic resonance imaging of 13 casesof supposedly malignant findings included in category 4, fourcases presented histopathological positive results formalignancy, showing 30.76% PPV. For the mammographic analysis of six cases of supposedly malignant findings included in category 5, all the cases presented histopathological positive results for malignancy, showing 100% PPV. For the sonographic analysis of 11 cases of supposedly malignant findings included in category 5, all the cases presented histopathological positive results for malignancy, showing 100% PPV. For the analysis by magnetic resonance imaging of 14 cases of supposedly malignant findings included in category 5, four cases presented histopathological positive results for malignancy, showing 92.85% PPV (Tables 2 to 4).
In a comparison between the different imaging modalities and the BI-RADS categories, one may observe high PPV in the three modalities for the category 5 (100% doe mammography, and 92.85% for magnetic resonance imaging). Magnetic resonance imaging presents a high NPV for category 3 (100%), while mammography and ultrasound present similar, intermediate PPV (respectively 69.23% and 70.58%). Additionally, the results demonstrate that the three imaging modalities presented intermediate PPV for category 4: mammography, 63,63%; ultrasound, 50%; and magnetic resonance imaging, 65.96% (Tables 2 to 4).
DISCUSSION As previously mentioned, BI-RADS category 3 includes lesionswith high probability of benignity. Notwithstanding the BI-RADSitself recommends not performing biopsy in patients with lesionsin category 3, this procedure is performed in a great number ofcases. The main factors influencing the biopsy practice are:patient's anxiety, physician's insecurity, and presence of riskfactor for breast cancer. The definition of BI-RADS categories 4 and 5 PPV, and category3 NPV would be a contribution to aid breast specialists in thedecision making about submitting patients to biopsies. Studies in the literature evaluating the predictive values ofthese BI-RADS categories for mammography cover all types ofnon-palpable breast lesions(14–16). In thesestudies, the NPV of category 3 ranged between 97% and 100%, whilethe PPV ranged between 23% and 34% for category 4, and between81% and 97% for category 5. Comparing the above mentioned results with those found by thepresent study exclusively about non-palpable breast masses, cleardifferences in predictive values are observed. Such differencesare particularly remarkable when BI-RADS category 3 isconsidered; in this category we have found a lower NPV. Thisdifference is explained by the fact that, because of theiretiological and morphological diversity, the greatest part ofcalcifications are classified as probably benign. Also, in the present study, with respect to category 4, wehave observed a higher PPV compared with those found by otherauthors. Considerable differences have not been found in PPV forcategory 5, considering that lesions in this category presenttypical features of malignancy in both groups, reducing thevariability in the images interpretation. Analyzing the sonographic findings in BI-RADS categories 3, 4and 5 as to their predictive value in relation to the malignantor benign nature of detected non-palpable breast masses, we haveobserved that the NPV of category 3 presented moderate levels;category 4, moderate PPV; and category 5, high PPV. Our resultsare similar to those presented by Hong etal.(9), emphasizing the capacity of predictingmalignancy in cases of non-palpable breast lesions evaluated byultrasound, if the BI-RADS is utilized, especially in thecategory 5. In our sampling, magnetic resonance imaging findingsclassified as BI-RADS categories 3, 4 and 5 were analyzed for aglobal evaluation of positive and negative predictive values.Correlating these findings with histopathological results frombiopsy specimens, we have concluded that PPV have shown to bemoderate for categories 4 and 5 as whole, while category 3 NPVand category 5 PPV have shown to be high. Our results weresimilar to those from the study developed by Gokalp andTopal(10) and Sadowski andKelcz(11). The present study, as well as other investigations developedemploying mammography, ultrasound and magnetic resonance imaging,is aimed at improving the prediction of malignancy or benignityof non-palpable breast lesions for a better management of thedisease and improvement of the biopsies practice. As regards category 4, the present study corroborates thesystematic necessity of biopsy for non-palpable breast masses,since the PPV observed for mammography, ultrasound and magneticresonance imaging was higher than those reported by theinternational literature covering all the types of abnormalmammographic findings(14–16). It is our opinion that the greatest contribution of thepresent study is related to non-palpable breast masses detectedby mammography, ultrasound and magnetic resonance imaging andclassified as BI-RADS category 3. Magnetic resonance imaging,because of the high NPV in this group of patients, should beconsidered as an important imaging method in the conservativemanagement of lesions classified as category 3, to avoidunnecessary biopsies, according to the results found both by thepresent study and Gokalp and Topal(10). Acknowledgement The authors thank the Núcleo de Apoio àPublicação da Faculdade de CiênciasMédicas da Santa Casa de São Paulo (NAP-SC), forthe technical-scientific support for publication of the presentstudy.
REFERENCES 1. Shapiro S. Determining the efficacy of breast cancer screening. Cancer 1989;63:1873–1880. [ ] 2. Dodd GD. American Cancer Society guidelines on screening for breast cancer. An overview. Cancer 1992;69:1885–1887. [ ] 3. Hurley SF, Kaldor JM. The benefits and risks of mammographic screening for breast cancer. Epidemiol Rev 1992;14:101–130. [ ] 4. Smart CR, Hartmann WH, Beahrs OH, Garfinkel L. Insights into breast cancer screening of younger women. Evidence from the 14-year follow-up of the Breast Cancer Detection Demonstration Project. Cancer 1993;72:1449–1456. [ ] 5. Nystrom L, Rutqvist LE, Wall S, et al. Breast cancer screening with mammography: overview of Swedish randomised trials. Lancet 1993;341: 973–978. [ ] 6. Smart CR. Highlights of the evidence of benefit for women aged 40-49 years from the 14-year follow-up of the Breast Cancer Detection Demonstration Project. Cancer 1994;74:296–300. [ ] 7. Hall FM, Storella JM, Silverstone DZ, Wyshak G. Nonpalpable breast lesions: recommendations for biopsy based on suspicion of carcinoma at mammography. Radiology 1988;167:353–358. [ ] 8. Breast Imaging Reporting and Data System (BI-RADSTM). 4th ed. Reston: American College of Radiology, 2003. [ ] 9. Hong AS, Rosen EL, Soo MS, Baker JA. BI-RADS for sonography: positive and negative predictive values of sonographic features. AJR Am J Roentgenol 2005;184:1260–1265. [ ] 10. Gokalp G, Topal U. MR imaging in probably benign lesions (BI-RADS category 3) of the breast. Eur J Radiol 2006;57:436–444. [ ] 11. Sadowski EA, Kelcz F. Frequency of malignancy in lesions classified as probably benign after dynamic contrast-enhanced breast MRI examination. J Magn Reson Imaging 2005;21:556–564. [ ] 12. Kopans DB, Lindfors K, McCarthy KA, Meyer JE. Spring hookwire breast lesion localizer: use with rigid-compression mammographic systems. Radiology 1985;157:537–538. [ ] 13. Rosner B. Fundamentals of biostatistics. 2nd ed. Boston: PWS Publishers, 1986. [ ] 14. Liberman L, Abramson AF, Squires FB, Glassman JR, Morris EA, Dershaw DD. The Breast Imaging Reporting and Data System: positive predictive value of mammographic features and final assessment categories. AJR Am J Roentgenol 1998;171:35–40. [ ] 15. Lacquement MA, Mitchell D, Hollingsworth AB. Positive predictive value of the Breast Imaging Reporting and Data System. J Am Coll Surg 1999;189:34–40. [ ] 16. Orel SG, Kay N, Reynolds C, Sullivan DC. BI-RADS categorization as a predictor of malignancy. Radiology 1999;211:845–850. [ ]
Received July 12, 2006.
* Study developed in the Department of Clinical Medicine and Department of Obstetrics & Gynecology of Faculdade de Ciências Médicas da Santa Casa de São Paulo, São Paulo, SP, Brazil. |
|
Av. Paulista, 37 - 7° andar - Conj. 71 - CEP 01311-902 - São Paulo - SP - Brazil - Phone: (11) 3372-4544 - Fax: (11) 3372-4554