Sr. Editor,
Paciente masculino, nove meses de idade, deu entrada na emergência por trauma do punho esquerdo. Após radiografia do antebraço ter mostrado fratura do rádio distal, foi feita imobilização do membro e encaminhado para acompanhamento ambulatorial. Após um mês, retornou com a mãe relatando emagrecimento e abaulamento da região após retirada precoce da imobilização. No exame físico observou-se edema pouco doloroso do terço distal do antebraço esquerdo, sem bloqueio articular do punho. Foram realizadas radiografia do antebraço (Figura 1A), ressonância magnética (Figuras 1B, 1C e 1D) e imobilização analgésica em tala axilopalmar associada a analgésico oral, com acompanhamento ambulatorial. Anatomopatológico conclusivo de tuberculose óssea e paciente em esquema terapêutico.
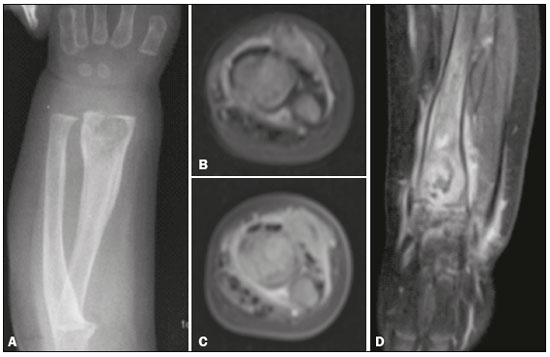 Figura 1. A:
Figura 1. A: Radiografia em anteroposterior do antebraço. Formação osteolítica, arredondada, margens parcialmente definidas, irregularidade da cortical e reação periosteal no terço distal do rádio.
B: RM axial DP. Lesão expansiva sólida heterogênea, limites imprecisos, ocupando a medular óssea da metáfise distal do rádio. Observa-se imagem linear hiperintensa no DP na metadiáfise e interrupção da cortical, sugestiva de fratura.
C: RM axial T1 com supressão pós-contraste. Sinal semelhante ao tecido cartilaginoso, com focos hiperintensos.
D: RM coronal T1 com supressão pós-contraste. A lesão ultrapassa focalmente a fise e infiltra partes moles perilesionais, com realce significativo pelo gadolínio, persistindo pequena loculações hipointensas; infiltração líquida e realce das interlinhas articulares, planos musculares e subcutâneo.
Atualmente, dois bilhões de pessoas encontram-se infectadas pelo
Mycobacterium tuberculosis e oito a nove milhões desenvolvem doença
(1). A tuberculose é um importante problema de saúde nos países em desenvolvimento. No Brasil, em 2012, foram registrados 71.230 casos novos, com taxa de incidência de 36,7/100.000 habitantes para todas as formas da tuberculose
(1-3). No mesmo ano, no Rio de Janeiro, foram registrados 10.871 casos novos
(1).
Após penetrar no organismo pela via respiratória, o
M. tuberculosis pode instalar-se em qualquer órgão, principalmente se houver queda da imunidade
(4). Existe maior dificuldade no diagnóstico das formas extrapulmonares, com confirmação bacteriológica em cerca de um quarto dos casos, em razão da localização das lesões e por serem paucibacilares. O estudo da imagem geralmente é inespecífico
(4).
A tuberculose óssea é uma doença incomum, acometendo 10-15% dos pacientes com tuberculose
(5-7). O envolvimento ósseo e articular é mais comum em crianças e idosos. Geralmente, é secundário a disseminação hematogênica, podendo ocorrer também por disseminação linfática ou por contiguidade
(4,5).
O esqueleto todo pode ser afetado, sendo a coluna o local mais comum e o rádio um local de acometimento raro. A clínica, em geral, manifesta-se por lesão monoarticular, sendo frequente o relato de traumatismo envolvendo a articulação afetada. Os achados radiográficos incluem lesões osteolíticas com irregularidade e esclerose circundante. As lesões ósseas com cavidade cística em radiografias são altamente inespecíficas e simulam osteomielite piogênica, infecção fúngica, metástase, osteossarcoma telangiectásico, cisto aneurismático, sarcoidose, granuloma eosinofílico ou cordoma
(8-10). Notavelmente, o diagnóstico é difícil por causa da sua natureza indolente e dos achados inespecíficos, acarretando aumento da morbidade e pior prognóstico
(4,6,11).
Concluindo, a tuberculose óssea, quando acomete locais incomuns, é de difícil diagnóstico e muitas vezes pode ser confundida com tumor, por apresentar semelhantes manifestações clínicas e achados de imagem. O médico deve estar sempre atento a possível causa pelo
M. tuberculosis, principalmente em áreas endêmicas, e ser cauteloso nos diagnósticos diferenciais, avaliando sempre a necessidade da biópsia, pois o tratamento tardio, ou excessivo, pode causar danos ao paciente.
REFERÊNCIAS1. Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Panorama da tuberculose no Brasil - indicadores epidemiológicos e operacionais. Brasília: Ministério da Saúde; 2014.
2. Hino P, Santos CB, Villa TCS, et al. O controle da tuberculose na perspectiva da vigilância da saúde. Esc Anna Nery. 2011;15:417-21.
3. Gupta P, Prakash M, Sharma N, et al. Computed tomography detection of clinically unsuspected skeletal tuberculosis. Clin Imaging. 2015;39:1056-60.
4. Lopes JA, Capone D, Mogami R, et al. Tuberculose extrapulmonar: aspectos clínicos e de imagem. Pulmão RJ. 2006;15:253-61.
5. Santos FCF, Nascimento ALA, Lira LAS, et al. Bone tuberculosis: a case report on child. Rev Soc Bras Med Trop. 2013;46:249-51.
6. Ye C, Hu X, Yu X, et al. Misdiagnosis of cystic tuberculosis of the olecranon. Orthopade. 2017;46:451-3.
7. Prakash J, Aggarwal S, Mehtani AK. Primary tuberculosis of the clavicle. Orthopedics. 2014;37:e879-84.
8. Sharma R, Gupta P, Mahajan M, et al. X-ray and computed tomography findings in macrodystrophia lipomatosa of the foot with secondary osteoarthritic changes diagnosed in an elderly female: a case report. Radiol Bras. 2017;50:132-4.
9. Reis LM, Duarte ML, Alvarenga SB, et al. Sarcoidosis: when the initial manifestations are musculoskeletal symptoms. Radiol Bras. 2018;51: 132-3.
10. Costa FM, Canella C, Vieira FG, et al. The usefulness of chemical-shift magnetic resonance imaging for the evaluation of osteoid osteoma. Radiol Bras. 2018;51:156-61.
11. Dhillon MS, Aggarwal S, Prabhakar S, et al. Tuberculosis of the foot: an osteolytic variety. Indian J Orthop. 2012;46:206-11.
1. Complexo Hospitalar de Niterói (CHN), Niterói, RJ, Brasil; a.
https://orcid.org/0000-0001-7883-88212. Complexo Hospitalar de Niterói (CHN), Niterói, RJ, Brasil; b.
https://orcid.org/0000-0002-0032-13283. Complexo Hospitalar de Niterói (CHN), Niterói, RJ, Brasil; c.
https://orcid.org/0000-0001-6265-53424. Complexo Hospitalar de Niterói (CHN), Niterói, RJ, Brasil; d.
https://orcid.org/0000-0002-3403-21535. Complexo Hospitalar de Niterói (CHN), Niterói, RJ, Brasil; e.
https://orcid.org/0000-0002-4682-7631Correspondência:
Dra. Vanessa Maria Terra Gomes
Complexo Hospitalar de Niterói
Rua La Salle, 12, Centro
Niterói, RJ, Brasil, 24020-096
E-mail:
nessa_terra@hotmail.comRecebido para publicação em 7/07/2017
Aceito, após revisão, em 11/08/2017

 |
|

